Migraines are not “just headaches.”
They are life-altering neurological events that steal time, energy, relationships, and joy — not only from the person suffering, but from the entire family around them.
Anyone who has lived in a household with migraines understands this. Plans are cancelled. Rooms go dark. Conversations go quiet. Children learn to tiptoe. Spouses learn helplessness. And the migraine sufferer, no matter how resilient or tough, carries an invisible burden that never truly lifts.
This is not theory for me.
It is personal.
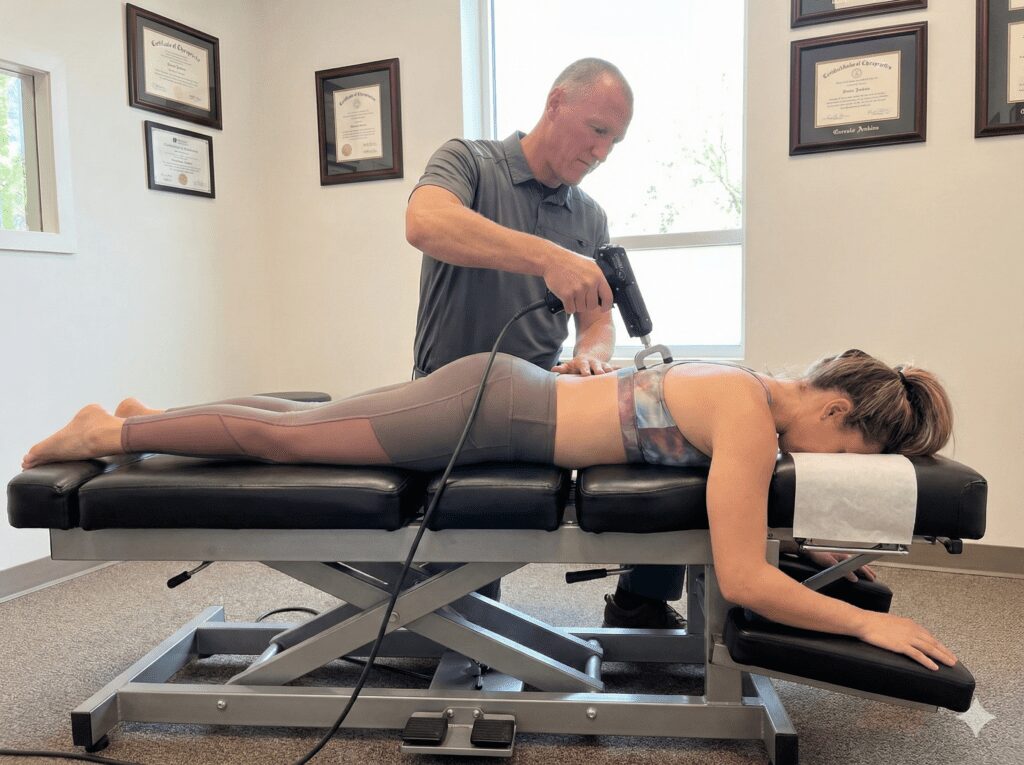
My passion for helping people with migraines began with my very first corrective case using Chiropractic BioPhysics® (CBP®) care — my own mother.
She had her first migraine at eight years old.
She had her last migraine at fifty-one.
That last migraine occurred three months after we began correcting the curve in her neck using CBP-based cervical spine correction.
After 43 years of migraines, they simply stopped.
That experience shaped the rest of my career. It forced me to ask deeper questions. It challenged everything I had been taught about migraines being purely chemical, genetic, or stress-driven. And it sent me down a path of studying posture, spinal alignment, neurology, and the growing body of chiropractic literature that connects cervical spine structure to migraine physiology.
This article is written for migraine sufferers, families, and clinicians who want more than symptom management. It is written for those asking a better question:
What if migraines are not random — but mechanical, neurological, and correctable?
Answering the core question first. . . .
Can chiropractic care — specifically CBP-based cervical spine correction — help migraines?
The evidence increasingly suggests yes, in the right patients.
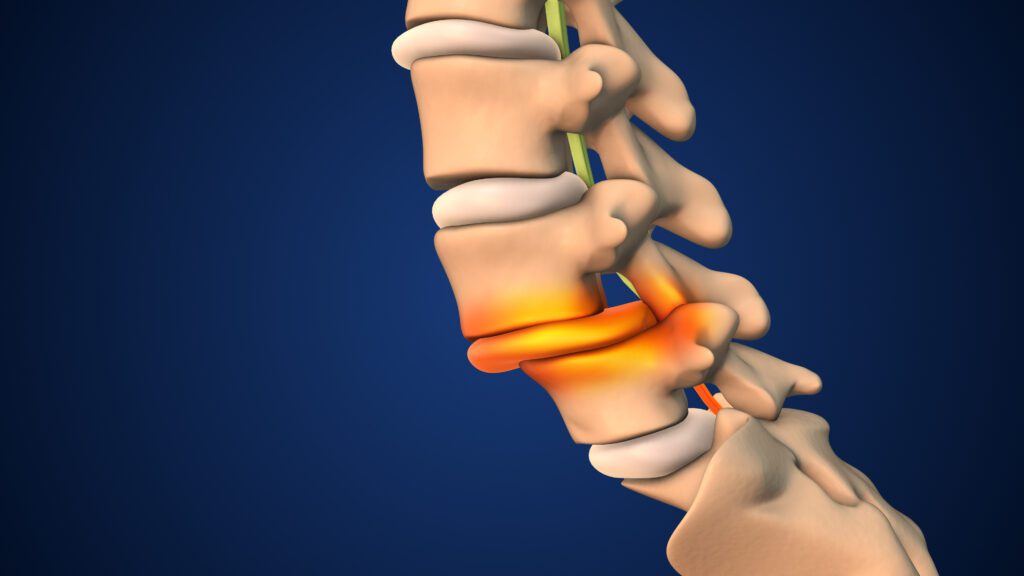
Migraines are complex neurological events involving the brainstem, trigeminal nerve system, blood flow regulation, muscle tension, and sensory processing. What is often overlooked is how strongly these systems are influenced by the alignment and function of the cervical spine.
Over the last 15–20 years, chiropractic research — particularly within the Chiropractic BioPhysics® (CBP®) model — has demonstrated that abnormal neck posture, especially loss of cervical lordosis and forward head posture, can place abnormal mechanical and neurological stress on the very structures involved in migraine generation [1][2][3].
When those structural problems are objectively identified and corrected, migraine frequency, intensity, and duration may significantly improve in selected patients [4][5].
This does not mean chiropractic “cures” migraines.
It means that for a subset of migraine sufferers — especially those with long-standing neck issues, posture changes, or trauma — structural correction may address a root cause that medications cannot.
The rest of this article explains why.
What a migraine really is (and why it’s so disabling)
Migraines are classified as a neurological disorder, not simply a pain condition. They often involve:
-
Severe, throbbing head pain (often one-sided)
-
Light and sound sensitivity
-
Nausea and vomiting
-
Visual disturbances (auras)
-
Neck stiffness or pain
-
Cognitive fog and fatigue
Modern research shows migraines involve abnormal sensory processing in the brainstem and trigeminal nerve system, altered blood vessel regulation, and heightened nervous system sensitivity.
But here’s the key point:
The upper cervical spine directly influences all of these systems.
The overlooked migraine–neck connection
Many migraine sufferers report neck pain before, during, or after an attack. For years, this was dismissed as a secondary symptom.
Today, we know better.
The upper cervical spine (C1–C3):
-
Houses and protects the brainstem–spinal cord junction
-
Influences blood flow to the brain
-
Is closely linked to the trigeminal nerve complex
-
Plays a major role in head posture and muscular balance
When cervical alignment is altered — especially with forward head posture and loss of the normal cervical curve — mechanical stress increases dramatically.
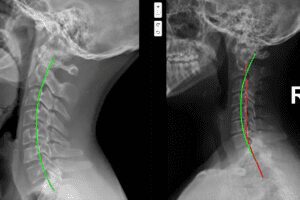
Research has shown that for every inch the head moves forward, the effective load on the cervical spine increases by approximately 10 pounds [6]. Over years or decades, this load changes muscle tone, joint mechanics, nerve signaling, and blood flow regulation.
This is not subtle.
And it is not benign.
Forward head posture: a silent migraine driver
Forward head posture (FHP) is now extremely common due to:
-
Screen use
-
Desk-based work
-
Mobile device habits
-
Early childhood posture changes
FHP alters the biomechanics of the cervical spine and increases tension in the suboccipital muscles — muscles that are richly connected to pain-sensitive neurological structures involved in migraines.
Multiple studies have demonstrated a strong association between migraine sufferers and abnormal head and neck posture [7][8].
Yet most migraine treatment plans never assess posture at all.
Why medications often fall short
Medications can be helpful. For some patients, they are essential.
But medications generally aim to:
-
Block pain signals
-
Alter blood vessel behavior
-
Suppress neurological excitability
They do not correct:
-
Abnormal spinal alignment
-
Mechanical stress on the cervical spine
-
Chronic postural distortion
-
Structural causes of neurological irritation
This is why many migraine sufferers cycle through medication after medication — often with diminishing returns.
The structure remains unchanged.
Chiropractic BioPhysics®: changing the diagnostic conversation
This is where Chiropractic BioPhysics® (CBP®) has fundamentally changed chiropractic care.
CBP introduced a higher diagnostic standard by emphasizing:
-
Objective spinal measurements
-
Postural analysis
-
Cervical spine radiographic assessment
-
Comparison to normal spinal alignment models
-
Repeatable re-examinations
Instead of asking only “Where does it hurt?”, CBP asks:
-
What is the shape of the cervical spine?
-
How far forward is the head?
-
How does this alignment affect neurological stress?
-
Can this structure be corrected?
These questions matter for migraines.
My mother’s case: why it changed everything
When my mother came under care, she had:
-
A 43-year migraine history
-
Migraines beginning at age 8
-
Decades of medical management
-
No lasting relief
What she also had — though no one had ever measured it — was significant cervical spine misalignment and loss of lordosis.
Using CBP protocols, we began gradual, corrective care aimed at restoring the normal curve in her neck.
Three months later, her migraines stopped.
No medication changes.
No lifestyle overhaul.
Just structural correction.
That experience aligned perfectly with what the emerging CBP literature was beginning to show.
What the research says about CBP and headaches
Over the past two decades, peer-reviewed chiropractic research has demonstrated:
-
Restoration of cervical lordosis can reduce headache frequency and intensity [4]
-
Long-term correction produces longer-lasting results than symptom-based care [5]
-
Structural changes correlate with neurological symptom improvement [2][3]
-
Posture correction affects nervous system function, not just pain perception [9]
Importantly, these improvements are often maintained after care ends, something rarely seen with purely symptomatic treatments.
Migraines, posture, and neurology: connecting the dots
When cervical alignment is corrected:
-
Mechanical stress on joints decreases
-
Muscle tone normalizes
-
Blood flow regulation improves
-
Trigeminal nerve irritation may reduce
-
Brainstem stress may decrease
This creates an environment where migraine triggers become less reactive.
Again, this does not apply to every migraine sufferer — but for the right candidate, it can be life-changing.
Why listening matters in migraine care
Migraines are deeply personal.
They are patterned.
They have histories.
A proper migraine assessment should explore:
-
Age of onset
-
History of falls or concussions
-
Childhood posture
-
Desk and device habits
-
Neck injuries
-
Symptom progression over time
CBP-based chiropractic care places heavy emphasis on history-taking, because structure changes slowly — and migraines often follow those changes.
Listening is not optional.
It is diagnostic.
Who may be a good candidate for CBP-based migraine care?
You may be a candidate if you:
-
Have long-standing or recurring migraines
-
Experience neck pain or stiffness with migraines
-
Have a history of head or neck injury
-
Spend long hours at a desk or on devices
-
Have never had your cervical spine posture measured
-
Have tried medications with limited success
A proper assessment is essential. Not everyone qualifies — and that honesty matters.
The role of corrective care vs. symptom relief
Traditional chiropractic care often focuses on short-term relief.
CBP-based care focuses on long-term structural correction.
This includes:
-
Specific spinal traction
-
Postural exercises
-
Mirror image® protocols
-
Measured progress over time
It requires commitment — but the potential payoff is profound.
Why families feel the difference
When migraines improve, families change.
-
Parents become present
-
Children feel safer
-
Partners stop waiting for the next attack
The ripple effect is enormous.
This is why migraine care must be taken seriously — and why structural approaches deserve attention.
A note for migraine sufferers
You are not weak.
You are not imagining this.
And you are not broken.
Your nervous system is responding to something — and in many cases, that “something” includes mechanical stress from poor cervical alignment.
Understanding that opens new doors.
Call to Action: start with a conversation
If you or someone you love suffers from migraines and you want to explore whether posture and cervical spine structure may be contributing, the first step is simple:
Book a complimentary consultation with the doctor to see if you may be a good candidate for today’s CBP-based chiropractic care at 100+Living Health Centres in Kelowna.
Take the Next Step
Don’t settle for temporary relief. Get care that helps correct the cause of your condition.
Step 1:
Start with a free 10-minute phone consult to discuss your symptoms and see if our approach is right for you.
Step 2:
Book your first comprehensive exam and consultation and get started.
This conversation is educational, pressure-free, and designed to help you understand your options — nothing more.
Final thoughts
Migraines steal decades from people’s lives.
They stole 43 years from my mother — and then they stopped.
That outcome shaped my purpose, my practice, and my belief that structural correction belongs in the migraine conversation.
If this article helps even one family reclaim their time, it has done its job.
References
-
Vernon H, McDermaid CS, Hagino C. Systematic review of randomized clinical trials of complementary/alternative therapies in the treatment of tension-type and cervicogenic headache. Complement Ther Med.
https://pubmed.ncbi.nlm.nih.gov/16105680/ -
Harrison DE, Cailliet R, Harrison DD, Janik TJ, Holland B. Reliability of centroid, Cobb, and Harrison posterior tangent methods. Spine.
https://pubmed.ncbi.nlm.nih.gov/9112707/ -
Harrison DD, Betz JW, Cailliet R, Harrison DE. Radiographic analysis of lumbar lordosis: centroid, Cobb, TRALL methods. Spine.
https://pubmed.ncbi.nlm.nih.gov/10209798/ -
Moustafa IM, Diab AA. The effect of adding forward head posture corrective exercises in the management of lumbosacral radiculopathy. J Chiropr Med.
https://pubmed.ncbi.nlm.nih.gov/25526965/ -
Moustafa IM, Diab AA. Extension traction treatment for patients with discogenic cervical radiculopathy. Clin Rehabil.
https://pubmed.ncbi.nlm.nih.gov/24413535/ -
Kapandji IA. The Physiology of the Joints, Volume 3: The Trunk and the Vertebral Column. Churchill Livingstone.
-
Fernández-de-las-Peñas C et al. Forward head posture and neck mobility in chronic tension-type headache. Cephalalgia.
https://pubmed.ncbi.nlm.nih.gov/16396602/ -
Fernández-de-las-Peñas C et al. Association between cervical posture and headache. J Manipulative Physiol Ther.
https://pubmed.ncbi.nlm.nih.gov/17046441/ -
Oakley PA, Harrison DE. Spinal alignment, posture, and neurological function. J Phys Ther Sci.
https://pubmed.ncbi.nlm.nih.gov/28626359/